In IVF treatment, most people focus on egg quality, sperm health, and embryo grading. While these are crucial, there is another equally important factor that often gets overlooked – the endometrium, or the lining of the uterus. For an embryo to successfully implant, the uterine lining must be healthy, receptive, and hormonally prepared. Even a high-grade embryo may fail to implant if the endometrium is not supportive.
This is why fertility specialists closely monitor endometrial thickness and blood flow during IVF cycles. Understanding the difference between a thin and thick endometrium – and how each affects implantation – can help couples make informed decisions on their fertility journey.
What Is the Endometrium and Why Is It Important in IVF?
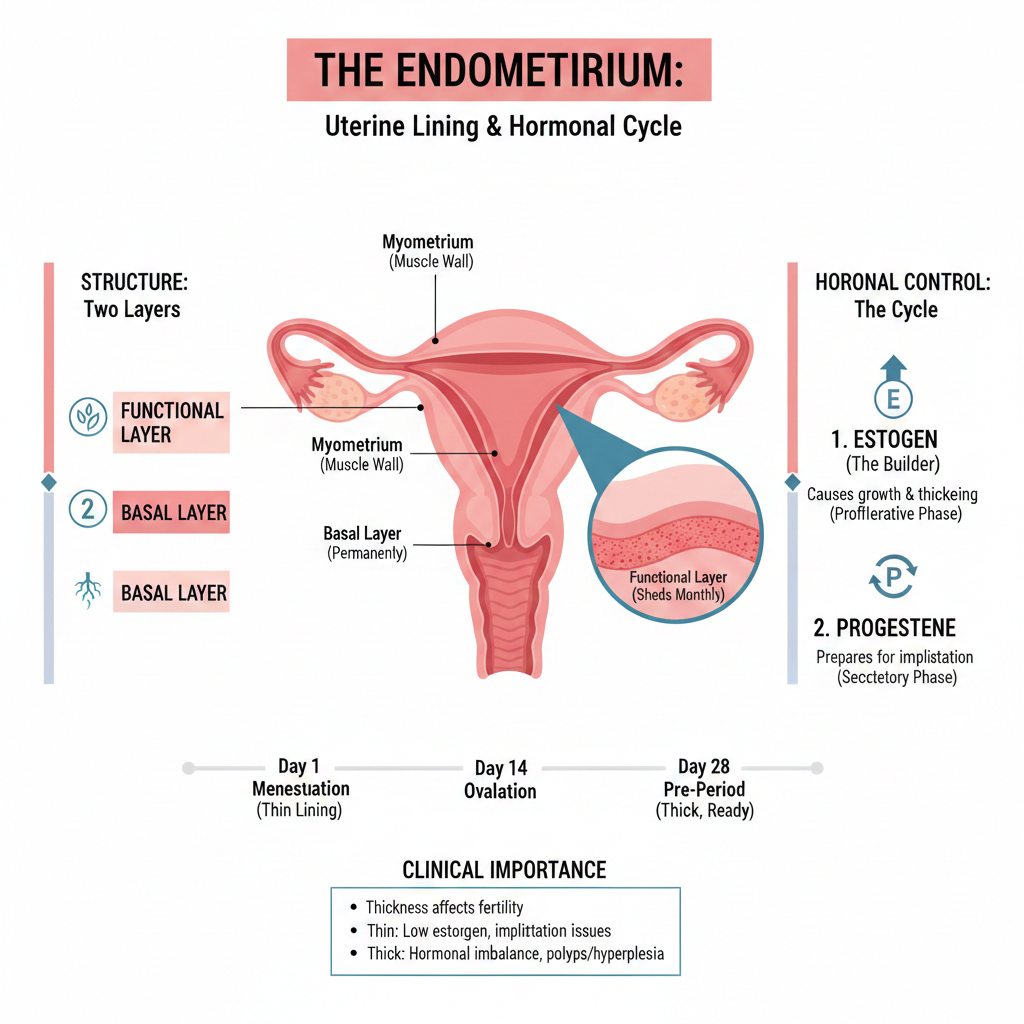
The endometrium is a soft, spongy layer inside the uterus. Its role is not only structural but also biological. During every menstrual cycle:
- After menstruation, estrogen helps the lining grow and rebuild.
- After ovulation, progesterone prepares it to welcome and nourish an embryo.
- If pregnancy does not occur, the lining sheds as menstrual blood.
In IVF, doctors schedule the embryo transfer when the endometrium enters its receptive phase, often called the “window of implantation.” During this window, the lining is thick, well-vascularized, and biologically ready for embryo attachment.
What Is a Thin Endometrium?
A thin endometrium usually refers to a lining below 7 mm around the time of embryo transfer. Although pregnancies can still occur, research shows that implantation rates are generally lower when the lining is very thin.
What Causes a Thin Lining?
A thin endometrium may develop due to:
- Low estrogen levels
- Hormonal imbalance
- Uterine infections
- Previous D&C or surgical trauma
- Endometrial scarring (Asherman’s syndrome)
- Long-term hormonal contraceptive use
- Smoking
- Poor uterine blood flow
- Diabetes or thyroid disorders
Some women notice light periods or short cycles, while others have no symptoms at all.
How a Thin Lining Affects IVF Implantation
Even when an embryo is genetically normal, it needs a thick and healthy lining to survive. A thin lining may lack:
- Adequate blood supply
- Proper nutrient support
- Receptive surface proteins needed for attachment
This can lead to implantation failure, biochemical pregnancies, or recurrent early miscarriages. For this reason, many clinics recommend thin endometrium treatment before transferring embryos.
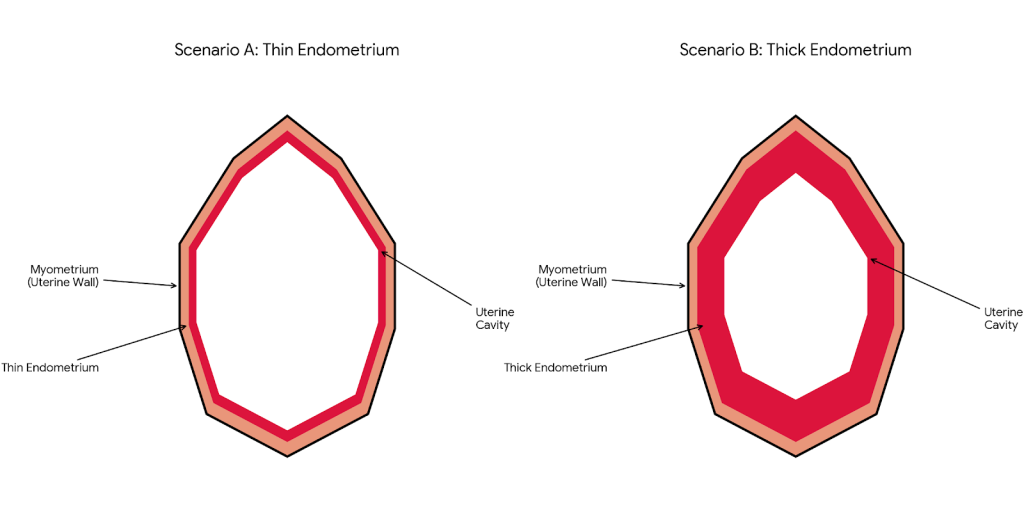
What Is a Thick Endometrium?
A thick endometrium generally measures above 12-14 mm. A thick lining is not automatically harmful, but problems may arise if it appears irregular or uneven. This can happen due to:
- Estrogen dominance
- Polycystic ovary syndrome (PCOS)
- Endometrial hyperplasia
- Polyps
- Fibroids
- Obesity
A thick lining may contain excess tissue that is not yet mature or receptive for implantation.
Is Thicker Always Better?
No. Studies show that both extremes – very thin or very thick – can reduce implantation chances.
The most successful IVF cycles usually have a lining that is:
- 8-12 mm thick
- Uniform
- With a trilaminar (triple-line) appearance
- Showing healthy blood flow on ultrasound
So, it is not the thickness alone, but the quality and structure that determine whether the endometrium is receptive.
Thin vs. Thick Endometrium: Which Improves Implantation?
The best outcomes occur when the endometrium is balanced: not too thin, not too thick, and hormonally synchronized with the embryo. A well-prepared lining provides nutrition, oxygen, and a stable environment where the embryo can implant and grow into a pregnancy.
For this reason, fertility experts monitor:
- Thickness
- Blood circulation
- Hormone levels
- Pattern (triple-line vs. homogeneous)
- Timing of progesterone exposure
- Structural abnormalities on ultrasound
When any of these factors are suboptimal, implantation becomes more difficult.
How Fertility Specialists Improve Endometrial Receptivity
1. Estrogen Therapy
When the lining remains thin, doctors often prescribe estrogen tablets, patches, gels, or injections. Estrogen thickens the lining and improves blood circulation. Regular scans track the response.
2. Progesterone Support
Even with a perfect lining, implantation will not happen without the right amount and timing of progesterone. This hormone stabilizes the lining, making it receptive. During IVF, progesterone levels are carefully managed to match the embryo’s stage.
3. Lifestyle and Blood Flow Improvements
Better blood flow brings oxygen and nutrients to the endometrium. Many specialists advise:
- Moderate exercise
- Hydration
- Avoiding smoking and alcohol
- Antioxidant-rich foods
- Managing thyroid and blood sugar levels
Some patients are prescribed low-dose aspirin or L-arginine to enhance uterine circulation.
4. PRP Therapy
Women with persistent thin lining may benefit from PRP for thin endometrium. PRP (Platelet-Rich Plasma) uses growth factors from the patient’s own blood to repair and regenerate uterine tissue. Many IVF centers use PRP when standard hormonal treatments are not enough.
5. Hysteroscopy
A hysteroscopy is a small endoscopic procedure that allows doctors to look inside the uterus. It can detect polyps, fibroids, adhesions, infections, or scarring that may interfere with implantation. Correcting these issues often improves IVF success.
6. Treating Underlying Conditions
If PCOS, thyroid imbalance, insulin resistance, or chronic inflammation is present, treatment can significantly improve endometrial development. Addressing root causes is often more successful than repeating IVF cycles without evaluation.
Does Endometrial Thickness Predict IVF Success?
A receptive lining is one of the strongest predictors of implantation success. Many women who experience repeated IVF failure later conceive after improving uterine conditions. For some patients, additional tests like ERA (Endometrial Receptivity Analysis) help determine the precise timing for embryo transfer.
IVF success is a combination of:
- Healthy embryo
- Proper hormonal environment
- Correct endometrial thickness
- Good blood flow
- Structural normality
A small change in endometrial health can make a big difference in pregnancy outcomes.
Conclusion
A successful IVF cycle is not only about fertilization and embryo development. The uterus must be ready to accept and support the embryo. A lining that is too thin may lack nutrients and blood supply, while one that is too thick may indicate hormonal imbalance. The ideal endometrium is balanced, well-vascularized, and hormonally receptive.
If a woman has experienced repeated implantation failure or unexplained IVF disappointment, evaluating the endometrium is a critical next step. With proper diagnosis, hormonal therapy, PRP treatment, or hysteroscopy, many women achieve better outcomes in future cycles.
If you are looking for the best IVF Center near you for expert endometrial assessment, IVF guidance, PRP therapy, and personalized fertility care, couples can consult Nishant IVF & Fertility Centre in Jaipur, where specialists work to improve implantation and make parenthood possible.
